Dar, you write: "I feel like i am so alone, left in limbo, i have no idea what lies ahead, what will my husband go through? "
Truthfully, while each patient is different, many diseases have a predictable trajectory. The reason for having 'staging' criterea and definitions is to allow primary care teams to perceive your situation and make the correct calls.
I have found, however, that many nurses (i'm not disparaging them, but they find palliative care difficult, as well) believe that it should be a secret amongst the clan.
Nurses and agencies are totally hampered by the government. They will give you the hand, but are having to spew policies. There are shortages of nurses (25%) and PSWs in Ontario, I'm sure across the continent. If you look in the want ads, you'll see ads all the time.
If you cannot cope, going to ER is the best place. They will get your spouse into a long-term care, or suitable placement before the CCAC will. There is no shame in being realistic in stating you are burned out. My late mother died on her couch, and I ended up on anti-depressants balancing my work and my caregiving. Dad died in LTC, peacefully, in a setting that wasn't ideal, but I was sleeping in the room beside him. The staff prepared me for 'the end', even though it was a lousy institution overall, and I wasn't alone.
If you want more information, read on:
I was at a workshop for PSWs and nurse training, as part of my volunteer training, and was curtly corrected. But I found that when caring for my father, these things helped me gain some understanding of how I can advocate and nagivate the end-of-life care that is required of us. When you do not feel you can cope anymore, there are hospices that will help. Both physical settings, and hospice volunteers, like myself, who will provide information and/or moral support.
Here are a couple of things that might help.
Firstly, ask your nurses (doctors are in denial) about the disease trajectory of your hubby. It helps build some perception into your caregiving assignment. It is something that has been a 'new' idea, and should not be a secret.
It's not being morbid. We are all going to die. Our disease governs our needs, symptoms, preparations, and pain management.
Some decline rapidly, others slowly, with recovery in between. Others decline in a stair-like deterioration. All are normal, depending upon the disease. Many are predictable, even if timelines differ.
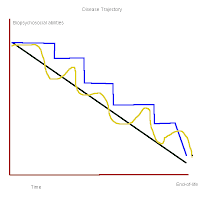 |
Disease Trajectory |
The 8 stages of chronic illness trajectory
1. Initial presentation of situation; occurs before any signs and symptoms of a disease
2. Trajectory onset
3. Crisis: potentially life-threatening situation
4. Acute: post crisis-symptoms controlled
5. Stable, symptoms are controlled
6. Unstable: e.g. foot ulcer,
7. Downward phase; progressive deterioration; mental & physical
8. Dying phase, weeks, days or hours preceding death.
Secondly, print these off, when you are ready, they will help you understand what is in the future:
There is no reason why these things should be secrets.
You are not alone. There are thousands of people in your situation, or have been in your situation.
You feel as if you are sitting, alone, in the dark, tyring to cope, when there are people who understand and are right next door to you.
No one told me about hospice volunteers. No one told me what to expect.
This is what I have learned, and I share with my caregivers who need the information.

The trajectory of a disease can be a gradual decline, or a series of declines, or a sudden decline in biopsychosocial symptoms. This means that a person with cancer will have a predictable decline in their physical (biological: mobility, food intake, awareness of their surroundings, ability to communicate, or to think abstract thoughts), psychological (mental acuity) and other behaviours. What often happens at end-of-life is that residents are unable to state their needs, whether it is to avoid food, limit liquids, refuse to be hauled out of bed three times a day, and to be left alone. Many at end of life prefer to be solitary, and quiet. Often soft music is an option. Peace and quiet, often missing in the noisy hallway of a LTC, is important for the resident.
Do not be afraid. You will be able to do all that is asked of you. You will not be asked to do more than you are able. You cannot make mistakes. You are decision-making for your loved one.
You are making decisions for your family and your family situation. Simply do the best you can, with the information you have on hand.
all the best.